Hand, Wrist, and Elbow Conditions Treated by Dr. Avery Arora
Dr. Avery Arora is a board-certified hand surgeon who specializes in diagnosing and treating conditions affecting the hand, wrist, and elbow. At Arora Hand Surgery, patients from across Metro Detroit seek care for carpal tunnel syndrome, trigger finger, arthritis, tendonitis, Dupuytren’s Contracture, tennis elbow, various injuries like fractures, tendon injuries, lacerations and other concerns that impact daily life.
Dr. Arora follows a patient-first philosophy that focuses on careful diagnosis and conservative treatment whenever possible. Many conditions affecting the hand and wrist can be treated without surgery. When surgical care is necessary, treatment plans are tailored to restore comfort, strength, and function.
The hand and wrist are complex structures made up of many small bones, tendons, ligaments, muscles, and nerves. When any of these structures become injured or irritated, it can lead to pain, numbness, weakness, or reduced mobility. Early evaluation by a hand specialist can help determine the cause of symptoms and identify the most appropriate treatment.
Below are several of the most common conditions treated at Arora Hand Surgery.
Carpal Tunnel Syndrome
Carpal tunnel syndrome occurs when the median nerve becomes compressed as it travels through the carpal tunnel in the wrist. This condition commonly causes numbness, tingling, weakness, or pain in the hand and fingers. Symptoms often worsen at night or during repetitive activities involving the hands.
Carpal tunnel syndrome is one of the most common nerve compression conditions affecting the upper extremities. Treatment may include wrist splinting, activity modification, injections, or surgical release when symptoms persist.
Learn more about carpal tunnel syndrome here.
Trigger Finger
Trigger finger occurs when inflammation narrows the tendon sheath that allows the finger to bend and straighten smoothly. As a result, the finger may catch, lock, or become painful when moving.
This condition is often associated with repetitive gripping activities and may also occur in patients with diabetes or certain inflammatory conditions.
Many cases of trigger finger can be successfully treated with corticosteroid injections or other conservative measures before surgery is considered.
Learn more about trigger finger treatment here.
Dupuytren’s Disease
Dupuytren’s disease is a condition that causes thickening of connective tissue in the palm of the hand. Over time, this thickened tissue may form cords that pull one or more fingers toward the palm.
Although the condition often progresses slowly, it can eventually interfere with hand function and daily activities. Treatment options vary depending on the severity of the contracture.
Learn more about Dupuytren’s disease here.
De Quervain’s Tendonitis
De Quervain’s tendonitis causes pain along the thumb side of the wrist due to inflammation of the tendons responsible for thumb movement. Patients may experience pain when gripping, pinching, or lifting objects.
This condition is commonly associated with repetitive hand movements and can often be treated with rest, splinting, therapy, or injections.
Learn more about De Quervain’s Tendonitis here.
Hand and Wrist Fractures
Fractures of the hand or wrist can occur due to falls, sports injuries, workplace accidents, or direct trauma. Proper diagnosis and treatment are important to ensure the bones heal correctly and to prevent long-term stiffness or reduced hand function.
Treatment may involve splinting, casting, or surgical repair depending on the severity and location of the fracture.
Learn more about factures here.
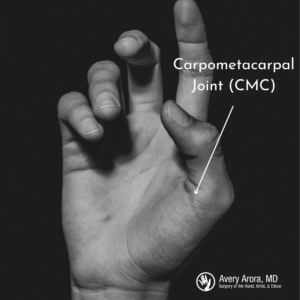
Thumb Arthritis
Arthritis at the base of the thumb is a common cause of hand pain, particularly in adults over the age of 40. This condition can lead to pain when gripping objects, reduced pinch strength, and difficulty performing everyday tasks.
Treatment may include splinting, medications, injections, therapy, or surgical options for more advanced cases.
Learn more about thumb arthritis here.
Cubital Tunnel Syndrome
Cubital tunnel syndrome occurs when the ulnar nerve becomes compressed at the elbow. This condition may cause numbness or tingling in the ring and small fingers, hand weakness, or difficulty with fine motor tasks.
Early evaluation can help prevent symptoms from progressing and identify the most effective treatment plan.
Learn more about cubital tunnel syndrome here.
Treatment Options
Treatment plans are carefully developed based on each patient’s condition, symptoms, and lifestyle. In many cases, non-surgical treatment can successfully relieve symptoms.
Common treatment options include:
- Hand therapy
- Splinting and bracing
- Corticosteroid injections
- Activity modification
- Pain management strategies
- Minimally invasive procedures
- Advanced hand surgery when necessary
Dr. Arora works closely with certified hand therapists to help patients regain strength, mobility, and function.
Procedures and Surgeries
Dr. Arora performs a wide range of surgical procedures involving the hand, wrist, and elbow. These procedures are designed to relieve pain, restore motion, and improve overall hand function.
Where Patients Can See Dr. Arora
Dr. Arora sees patients at several convenient Arora Hand Surgery locations throughout Metro Detroit, Michigan including:
- West Bloomfield
- Macomb
- Howell
Patients searching online for a hand surgeon near Metro Detroit often visit one of these locations for expert evaluation and treatment of hand, wrist, and elbow conditions.
Schedule an Appointment
If you are experiencing pain, numbness, weakness, or limited motion in your hands, wrists, or elbows, evaluation by a hand specialist may help determine the cause and appropriate treatment.
Dr. Avery Arora and the team at Arora Hand Surgery are committed to providing thoughtful, patient-centered care.
Contact Arora Hand Surgery today to schedule an appointment.